- Be able to distinguish successive parts of the circulatory pathway, and explain how the structure of the vessel wall meets the functional needs that are present in each of the parts.
- Know how structural differences in capillaries influence the passage of diverse material across the endothelium.
- Recognize features in the heart (such as cardiac muscle, valves, cardiac skeleton) that allow it to serve as a pump.
- Be able to describe the path of the cardiac impulse from sinoatrial node to the ventricle, and recognize the cells in the ventricle that are involved
A. Muscular (medium) Artery and Vein
Slide 30 Mesentery, H&E View Virtual Slide
Slide 42 Mesentery, H&E View Virtual Slide
Slide 95M Mesentery, trichrome stain View Virtual Slide
Slide 303 Artery & vein, Verhoeff stain [elastic fibers stain purple] View Virtual Slide
Slide 304 Femoral artery & vein, canine, van Gieson stain [elastic fibers stain brown] View Virtual Slide
Additional slides (not referenced below, but they show more examples of muscular arteries and veins):
Slide 95 Mesentery, H&E View Virtual Slide
Slide 92 Artery & vein, H&E View Virtual Slide
Slide 92F Femoral artery & vein, canine, trichrome stain View Virtual Slide (same as 304 above, but trichrome-stained)
Study the arteries first in slide 30 View Image, slide 42 View Image, and/or slide 95 (trichrome) View Image. Technically, these vessels are actually "small" arteries rather than "medium" arteries (the only difference is that medium arteries usually are given all those pesky anatomy names like "left pericardiacophrenic artery" whereas small arteries are not named). You do NOT need to worry about distinguishing between small and medium arteries histologically, but you should be aware of the organization of the typical muscular artery, of which these are excellent examples. Note the thin intima, the distinct internal elastic lamina (IEL) and the media composed of smooth muscle cells. The media also contains some elastin and abundant "reticular" collagen, as well as specific proteoglycans. There is sometimes a condensation of elastic fibers in the outer portion of the media that may be an "external elastic lamina", which varies from artery to artery. The adventitia is the dense, irregular connective tissue surrounding the media. Remember that in blood vessels the components of the media are arranged circularly, while those of the adventitia are oriented longitudinally. In vessels where the media is too thick to be supported by simple diffusion, vasa vasorum (e.g. shown here in slide 95M) may also be observed in the adventitia.
The structure of the companion veins in slide 30 View Image , slide 42 View Image , and/or slide 95 (trichrome) View Image is much less regular and may be difficult to understand at first, but still consists of the same basic layers as arteries with a tunica intima, media, and an adventitia, although the media is usually much thinner compared to the companion artery. Conversely, the adventitia is usually thicker in veins and may often have some bundles of longitudinal smooth muscle View Image as well as vasa vasorum View Image . In some sections, you may be able to see a thin internal elastic lamina beneath the venular endothelium (particularly in slide 95M). While the presence of such a structure is not common, it can be found occasionally in some veins, so don't use the presence or absence of an IEL as the sole diagnostic criterion for an artery, but in addition consider how well it is developed.
Slides 303 and 304 are of actual medium (i.e. named) arteries and veins. The artery in slide 303 View Image exhibits some intimal thickening (the endothelium is not evident, but you can see a crescent of tissue in between the IEL and the lumen on the right side of the artery) and deep purple-staining elastic fibers of the IEL and within the media can be readily seen. The vein in slide 303 View Image is irregularly shaped and also shows some intimal thickening. The media is thinner compared to the artery whereas the adventitia is a bit thicker --several vasa vasorum may also be seen. The "loose" appearance of the connective tissue in the adventitia is an ARTIFACT of specimen preparation --in reality, the adventitia is a sheath of dense irregular connective tissue. In slide 304, the elastic lamellae (they look like "fibers," but they are actually sheets of elastin --you're just looking at them edge-on) in the tunica media of the artery View Image appear brown-black whereas all of the cells and collagen fibers are stained with eosin (no hematoxylin was used, so no nuclei can be seen) allowing you to again see the distribution of elastic tissue in the IEL, the media, and the adventitia. The vein in slide 304 has been sectioned at a point where it is joined by a tributary, so it is a bit difficult to make out the layers in some places, but if you look in the area right next to the artery, you'll see a relatively thin media (the endothelium is not that evident) and an extensive adventitia. At the junction where the tributary empties into the femoral vein, there are two valve leaflets View Image , which are extensions of the intima. You may also notice that there are more elastic fibers on the side of the valve facing the blood flow which helps the valve close to prevent backflow.
B. Small Arteries and Veins
Slide 30 Mesentery, H&E View Virtual Slide
Slide 40 Trachea, H&E View Virtual Slide
Slide 42 Mesentery, H&E View Virtual Slide
Slide 93 Mesentery, H&E View Virtual Slide
Slide 95M Mesentery, trichrome stain View Virtual Slide
In addition to the small arteries and veins in slides 30, 42, and 95, you should also look for arterioles and venules View Image. Side-by-side examples present are excellent. Side-by-side comparisons of wall thickness rather than luminal diameter is usually a better way to differentiate arteri(es/oles) from veins/venules as the apparent diameter may be vary with the plane of section (an obliquely sectioned arteriole may appear to have a larger lumen than a companion venule cut in cross section). Many of the rather large vein-like vessels in slide 30 are actually very large lymphatic vessels View Image, some of which contain easily recognizable valves. These large lymphatic vessels may be differentiated from veins by the conspicuous ABSENCE of red bloods cells (lymph vessels usually contain ONLY white blood cells). In slide 40 of the trachea, arterioles and venules View Image may be found in the connective tissue between the respiratory epithelium and the numerous glands. Slide 93 offers an opportunity to look at a small artery View Image and vein View Image in longitudinal section.
C. Capillaries and Lymphatics
Slide 98HE Heart wall, H&E View Virtual Slide
Slide 98-N Heart wall, trichrome stain View Virtual Slide
Slide 102 Hear, left ventricle wall, H&E View Virtual Slide
Slide 305 Heart wall, H&E View Virtual Slide
Slide 29 Small intestine, H&E View Virtual Slide
The myocardial connective tissue of the heart (especially in the ventricles) in slides 98, 102, and 305 contains excellent examples of capillaries in various planes of section. With a little looking you'll find a circular endothelial cell sometimes with a single red blood cell View Image contained within the lumen. Find several examples.
As you have seen in the mesentery samples above (slides 30, 42, 93, and 95), lymphatic vessels of varying size can be found in association with nearby lymph nodes. However, these channels are also present in just about every other organ. Slide 29 of the small intestine is a good example in which lymphatics may be seen in the connective tissue in the wall of the gut tube (example). The main identifying feature of lymphatic vessels is that they usually have a VERY thin wall compared to the lumen.
D. Aorta
Slide 36 Aorta, aldehyde fuchsin stain View Virtual Slide
Slide 88 Aorta, H&E View Virtual Slide
Look at both stains. Note that a precise junction between the intima and media is not easy to recognize in either the trichrome View Image or H&E-stained View Image sections. Unfortunately, the endothelial layer is mostly absent in both slides. The transition from the media to adventitia, however, can be easily recognized in both trichome View Image and H&E-stained View Image sections. The trichrome and even the H&E stain visualizes the high concentration of elastic fibers in the tunica media. These elastic fibers and other extracellular matrix molecules are secreted by the resident smooth muscle cells in the wall of the aorta (NOT by fibroblasts which are not found in the tunica media).
NOTE: The radial folds [see orientation] in these sections are artifacts (folds) due to the elastic nature of the vessel and are not vasa vasorum, although examples of these small vessels may be found usually at the transition from the media to adventitia (look for spaces containing RBCs) View Image.
E. Large Veins
Slide Drexel University MCP35 Inferior vena cava, 20X H&E View Virtual Slide (virtual slide courtesy of Drexel University)
The Drexel University slide MCP35 shows the wall of a large vein, the inferior vena cava. Note the longitudinally-oriented bundles of smooth muscle cells in the tunica adventitia.
A. Heart wall
Slide 98HE Heart wall, right atrium & vent, H&E View Virtual Slide
Slide 98-N Heart wall, right atrium & vent, trichrome stain View Virtual Slide
This section is stained either with H&E or with Aldehyde Fuchsin-Masson. You should look at both stains. Locate the atrioventricular sulcus that contains a branch of the coronary arterial system (a muscular artery that exhibits moderate intimal thickening) embedded in theepicardial fat. Look at the connective tissue present between the ventricle and atrium. This is part of the cardiac skeleton into which cardiac muscle inserts. A leaflet of an A-V valve takes origin from the cardiac skeleton. Look at the atrial and ventricular endocardium. In some areas the endothelium has been lost during the preparation of the slide. In this section use the endocardium just superior to A.V. sulcus as "typical" atrial endocardium. With low power, locate the Purkinje fibers present immediately beneath the ventricular endocardium in the H&E View Image and trichrome-stained View Image sections (note the appearance of these fibers in cross and longitudinal orientations). These conducting fibers are larger and paler staining than the cardiac muscle fibers. Note the arrangement of the cardiac muscle (myocardial) fibers and the investing connective tissue.
B. Interventricular septum and valves
Slide 99HE Heart septum, H&E View Virtual Slide
Slide 99HM Heart septum, H&Masson stain View Virtual Slide
Slide 99M Heart septum, trichrome stain View Virtual Slide
The interventricular septal connective tissue is present, and, in most sections, a distinct unit of specialized cardiac muscle, the A-V bundle (of His), traverses the septal connective tissue (a thin group of muscle fibers surrounded by dense c.t.). The A-V bundle is easiest to see in slide 99HM, View Image , although although you should also be able to recognize it the H&E-stained section View Image as well. In these slides, the bundle fibers are cut in cross section and they are similar in size and staining to that of normal cardiac muscle fibers, although in some of your sections the fibers may more closely resemble Purkinje fibers (which is what they are). On one side of the section, a leaflet of the aortic valve View Image is present. On the other side, portions of an A-V valve View Image are present, as are bits and pieces of collagenous chordae tendinae. In slide 99HE, there is a piece of chorda tendinae actually attached to the valve View Image, whereas in slide 99M, the pieces are unattached and out in the ventricular lumen (the attachment site is out of the plane of section View Image.
C. Heart aortic valve
Slide 100HE Heart, left ventricular wall, H&E View Virtual Slide
Slide 100W Heart, left ventricular wall, Weigert's aldehyde fuchsin stain View Virtual Slide
Slide 100HM Heart, left ventricular wall, H&Masson stain View Virtual Slide
Slide 102 Heart, left ventricular wall, H&E View Virtual Slide
There are 3 stains for this section (H&E, aldehyde fuchsin only, mislabeled Masson, and Masson with hematoxylin counterstain, labeled H & Masson). Note the histology of the semilunar valve and the wall of the aorta View Image at the root of the aorta, both of which may be seen in close association with the fibrous cardiac skeleton. Check the heart slide 102. This H&E stained section provides another good histological study of the heart including part of the aortic valve.
120 Left Atrioventricular Valve - Bicuspid or Mitral Valve Atrioventricular Valve View Virtual EM Slide
Note that the valve is composed of two apposing layers of endocardium. The core of the valve contains loose connective tissue near the surface of the atrioventricular orifice and a thick, dense connective tissue plate on the opposite side. Note the absence of smooth muscle cells or capillaries within the substance of the valve. What covers the valve leaflets? (CV5) PATHOLOGY: The small dense spherules in the connective tissue represent the beginning of a calcification process - an aging phenomenon.
339 Chorda tendinae - Cross Section of Left Ventricle View Virtual EM Slide
Chorda Tendinae. In this electron micrograph, study the arrangement of collagenous and elastic fibers in this small tendon. The endocardium is reduced to the layer of endothelial cells. Where are the cardiac muscle fibers? (CV6)
96 Artery - Cross Section; Elastic Type Elastic Artery VIew Virtual EM Slide
Elastic Artery. Note the alternating layers of connective tissue and smooth muscle cells in the media. If there are no fibroblasts in the media, which cell is involved in the synthesis and maintenance of the collagen and elastic fibers as well as vascular proteoglycans? (CV7) The junction between the intima and media is difficult to identify!
97 Renal artery - Muscular Artery View Virtual Slide
Muscular Artery. Note that the intima in this type of artery consists of only the endothelium. Note also, the obvious internal elastic lamina, the paucity of elastic components within the media and the arrangement of smooth muscle cells.
101 Arterioles View Virtual EM Slide
Note that the media in an arteriole consists of only one or two layers of smooth muscle cells. An adventitia may not be present. CAUTION: Although this arteriole contains a complete, albeit thin, internal elastic membrane, many arterioles do not.
98 Small vein View Virtual EM Slide
In this wall of a vein, the tunica intima (endothelium), tunica media (3 layers of smooth muscle and interspersed elastic fibers) and a portion of tunica adventitia (collagen fibrils) are clearly recognized.
114 Continuous Capillary View Virtual EM Slide
Note abundance of micropinocytotic vesicles.
116 Continuous Capillary - Blood-Brain Barrier View Virtual EM Slide
Note the lack of vesicles, a reflection of a true blood-brain barrier. Remember that tight junctions restrict the transendothelial passage of metabolites and fluid.
119 Fenestrated Capillary View Virtual EM Slide
Note the diaphragms within the fenestrations.
110 Postcapillary Venule View Virtual EM Slide
This is an electron micrograph of a portion of a microcirculatory bed. Observe the addition of pericytes to the wall of the venous capillary (those capillaries that empty into venules) and the postcapillary venule - as opposed to the situation in true capillaries. (You do not have to distinguish subtle differences in microcirculatory bed structure!). Remember that this is the segment of the microvascular bed where lymphocytes and polymorphonuclear leukocytes exit the vascular systems by traversing the vessel wall by the process of diapedesis.
Click on a question to reveal the answer.
What kinds of cells are found in the aortic media?
Mostly smooth muscle cells. These are specialized smooth muscle cells that are responsible for the synthesis of collagen and elastic fibers in the media (these substances are not produced by fibroblasts in the aortic media). The collagen fibrils of the media and intima are of smaller diameter (30nm) than those in the adventitia, which are the products of fibroblasts. The individual smooth muscle cells in the media are enveloped by a typical basal lamina and have gap junctions with neighboring cells. These low-resistance junctions are essential for coordination of muscle contraction throughout the tunica media.
What is the composition of the AV valve?
The AV valve is avascular and is mostly made up of collagen and elastic fibers that are covered by an endothelium. As with all valves, there are more elastic fibers on the side of the valve that faces the blood flow, helping it return to its original shape and position. In the case of the AV valve, elastin is most abundant on the atrial side of the valve.
What is the distribution of elastin in the aortic valve?
In the aortic valve, there is more elastin on the ventricular side (see reasoning in CV2).
Is there a difference in endocardial thickness between the atria and ventricles?
Yes. Although it is not very clear in your slide collections, the endocardium is thicker in the atria than in ventricles. The atrial endocardium also contains more collagen and elastic fibers than does the endocardium of the ventricle and this connective tissue reinforces the relatively thin atrial myocardium.
What covers the valve leaflets?
Cardiac valves are avascular tissues covered by an endothelium.
Where are the cardiac muscle fibers in the chordae tendinae?
Trick question. There is no cardiac muscle in the chordae. They are collagenous strands that connect the valve leaflets to the papillary muscles, which are composed of normal cardiac muscle cells and Purkinje cells.
Which cell is involved in the synthesis and maintenance of the collagen and elastic fibers as well as vascular proteoglycans in the aorta?
In the aorta, as in all arteries, smooth muscle cells in the tunica media play this crucial role.
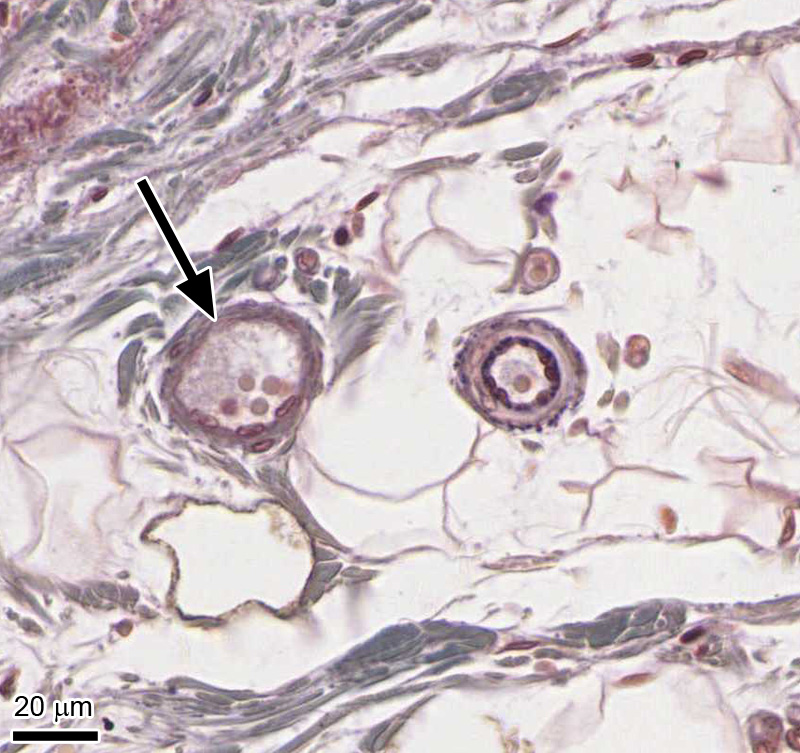
1. Identify the vessel that is indicated by the black arrow.
- Muscular artery
- Mid-size vein
- Arteriole
- Venule
- Capillary
Answer
Correct answer 4. A venule. Note the size of the vessel (compared to the erythrocytes it contains) and the relative thinness of the vessel wall. Also a comparison with the nearby arteriole identifies it as a venule.
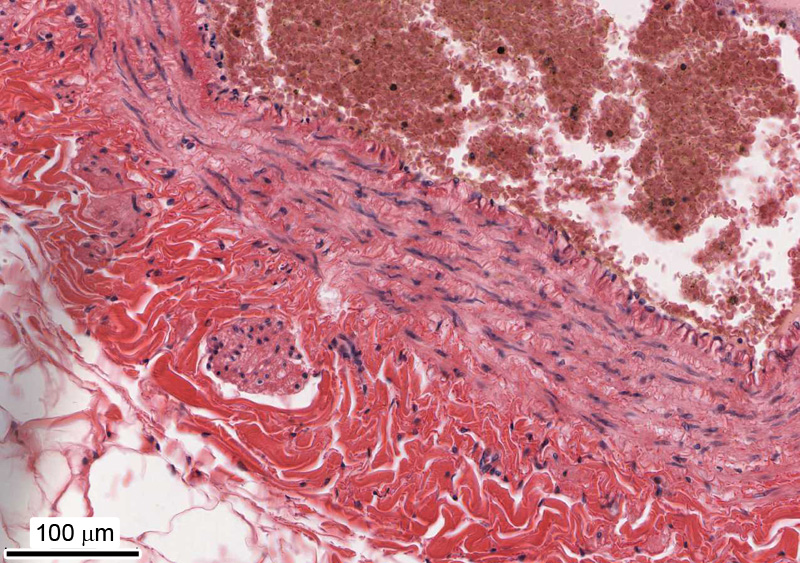
2. The image shows the wall of a component of the cardiovascular system. Identify this component.
View Image
- Heart ventricle
- Heart atrium
- Muscular artery
- Elastic artery
- Mid-size or large vein
- Large lymphatic vessel
Answer
Correct answer 5. This is a mid-size or large vein. Note the cross section of a longitudinal smooth muscle bundle in the tunica adventitia.
3. Select the correct statement(s) describing the group of cells indicated by arrow.
View Low Resolution Image
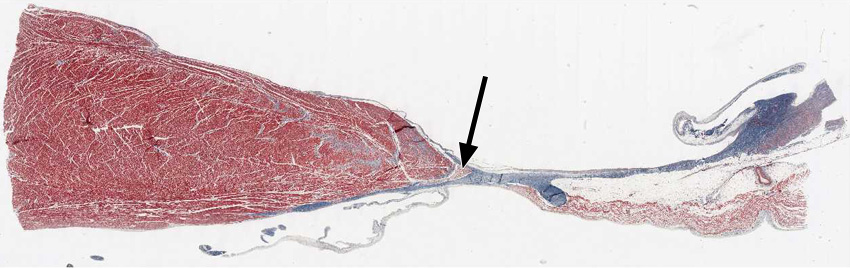
View High Resolution Image

- They synthesize and maintain components of the cardiac skeleton.
- They initiate contraction of atrial myocardium.
- They attach to atrioventricular valve leaflets via chorda tendinae.
- They conduct action potentials from the A-V node to the ventricular myocardium.
- They contract vigorously when stimulated and therefore contributes significantly to overall cardiac output.
Answer
Correct answer 4. Indicated is the AV bundle or bundle of His. It conducts the action potential from the A-V node to the ventricular myocardium.
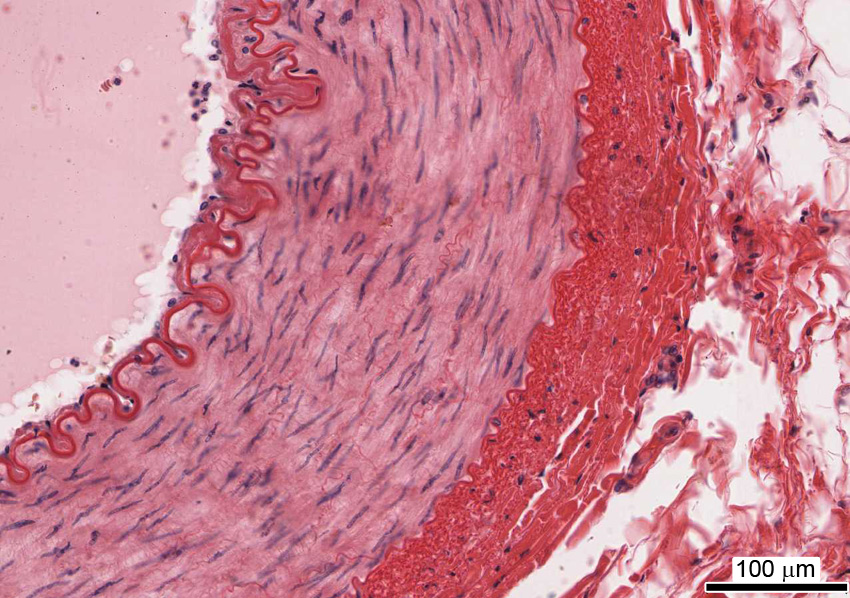
4. The image depicts the wall of a cardiovascular component. Identify that component.
View Image
- Heart ventricle
- Heart atrium
- Muscular artery
- Elastic artery
- Mid-size or large vein
- Large lymphatic vessel
Answer
Correct answer 3. Muscular artery. Note the well-defined inner elastic lamina and the thickness of the smooth muscle layer forming the tunica media.
5. This TEM micrograph depicts an A-V valve leaflet. Which bar/letter marks the endocardium?
View Image
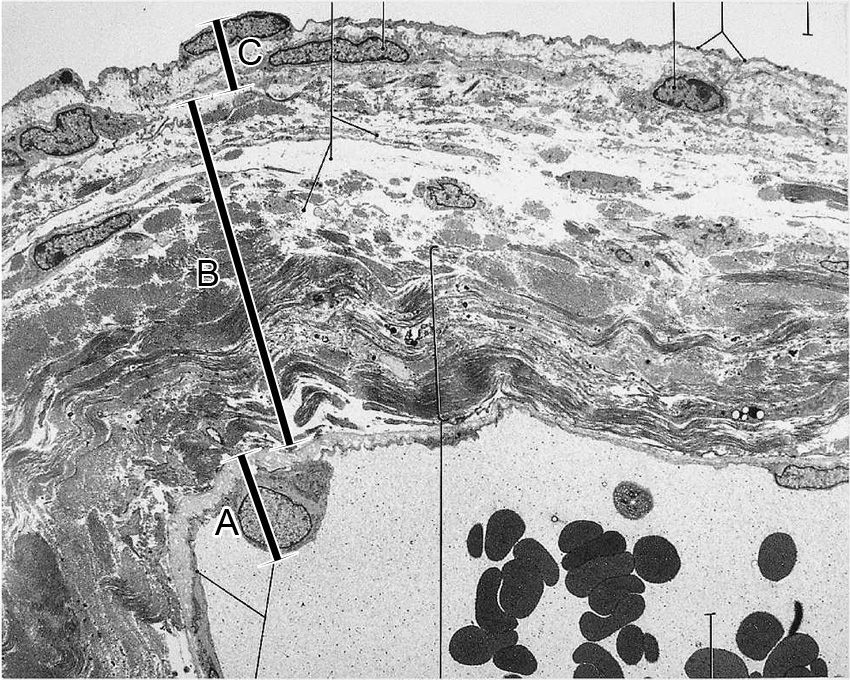
- Bracket A
- Bracket B
- Bracket C
- Brackets A and B
- Brackets A, B, and C
Answer
Correct answer 5. Brackets A, B, and C. As a heart valve leaflet is formed by a fold of the endocardium, the entire AV valve is part of the endocardium.
6. Which statement regarding vascular smooth muscle cells is NOT true?
- They are especially abundant in the tunica intima of some mid-size blood vessels.
- They produce reticular and elastic fibers in the tunica media of large elastic arteries.
- If present in the tunica media of any blood vessel, they are oriented circularly.
- They may be present as longitudinal bundles in the tunica adventitia of large veins.
Answer
Correct answer 1. Smooth muscle cells are not found in the tunica intima.
7. Identify the molecular components that form the structure that is indicated by the arrow in the TEM.
View Image
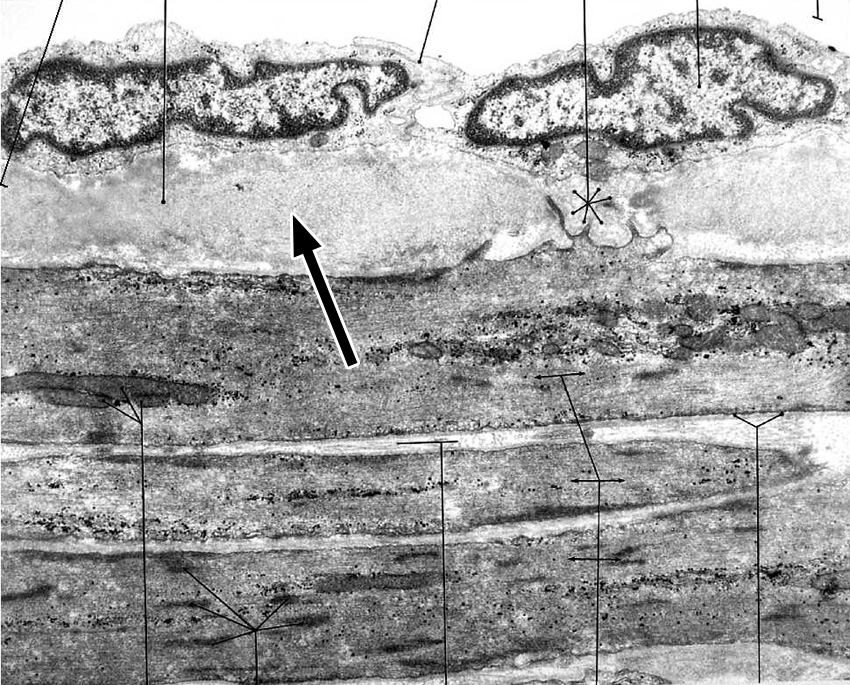
- Type IV collagen and laminin
- Elastin and fibrillin
- Type I collagen
- Smooth muscle cell cytoplasm
- Endothelial cell cytoplasm
Answer
Correct answer 2. Elastin and fibrillin. Most likely this image depicts the inner elastic lamina (IEL) of a muscular artery.
8. In this section of heart tissue, which of the brackets correctly demarcates the endocardium?
View Image
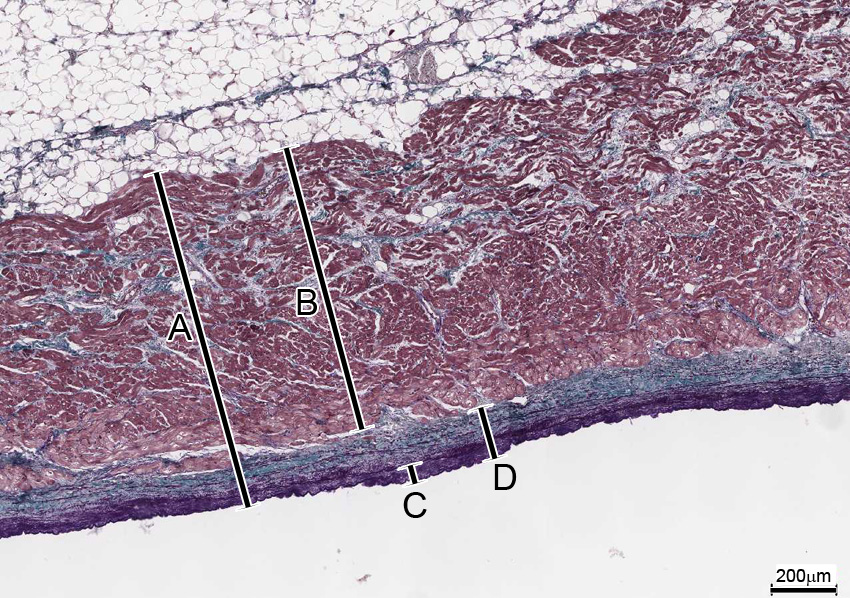
- A
- B
- C
- D
Answer
Correct answer 4. (D)